When your nails start looking wrong-yellow, thick, crumbly, or lifting away from the skin-it’s easy to assume it’s just a fungal infection. But what if it’s not? In fact, nearly one in ten people worldwide deals with nail changes that look similar but have completely different causes. Two of the most common culprits are fungal nail infections and nail psoriasis. They both cause discoloration, thickening, and detachment. But the treatments? Totally different. Get one wrong, and you could waste months, spend hundreds of dollars, and make things worse.
What’s Really Going On Under Your Nails?
Nail psoriasis and fungal infections might seem like twins, but they’re not. Nail psoriasis is an autoimmune condition. Your immune system, for reasons we don’t fully understand, starts attacking the nail matrix-the tissue under your cuticle where nails grow. This triggers skin cells to multiply way too fast. Instead of taking 28 to 30 days to reach the surface like normal skin, they rush up in just 3 to 4 days. That buildup doesn’t just show up on your elbows or knees-it shows up under and around your nails. Fungal nail infections, or onychomycosis, are caused by fungi. The most common offender is Trichophyton rubrum, which accounts for 80 to 90% of cases. These fungi don’t invade your body. They live in warm, damp places-like your shower, your socks, your gym shoes-and they latch onto your nails when they’re exposed. Once there, they feed on keratin, the protein nails are made of. That’s what causes the crumbling, thickening, and darkening.The Telltale Signs: Pitting, Odor, and More
Here’s where you start to see the difference. Nail psoriasis doesn’t just change the color. It changes the structure. Look for:- Nail pitting: Tiny dents or holes in the nail surface. Found in 70% of cases. This is one of the most reliable signs of psoriasis. You won’t see this with fungus.
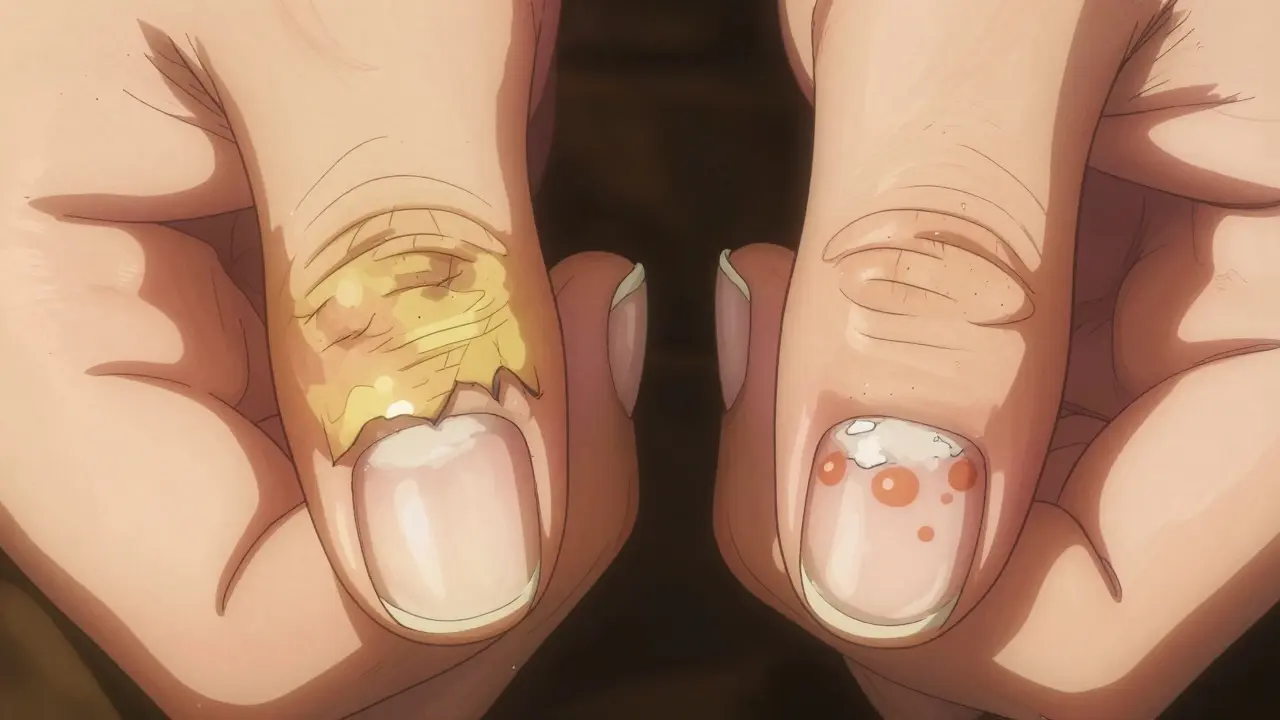
- Salmon patches: A translucent red or yellow discoloration under the nail. It looks like a drop of oil-hence the name “oil-drop lesions.” This happens in 15 to 50% of psoriasis cases.
- Onycholysis: The nail lifts away from the nail bed. Happens in 55% of psoriasis patients. It’s often uneven, with multiple nails affected at once.
- Subungual hyperkeratosis: A chalky, white buildup under the nail. It’s thick and crumbly, not just discolored.
Fungal infections, on the other hand, follow a pattern:
- Thickening: Nails get noticeably thicker-often 3 to 5 mm. Psoriasis thickens too, but usually less, around 2 to 3 mm.
- Color change: Starts as a white or yellow spot under the tip, then turns brown or black as it spreads. Fungal nails almost always darken.
- Foul odor: Present in 40% of fungal cases. Psoriasis? Zero odor. If your nail smells bad, it’s a strong clue it’s fungal.
- Starts at the edge: Fungus usually begins at the side or tip of the nail and creeps inward. Psoriasis often hits multiple nails at once, including fingernails.
And here’s a key point: 78% of people with nail psoriasis already have skin psoriasis. If you’ve had plaques on your elbows or scalp for years, and now your nails are acting up, it’s likely psoriasis. Fungal infections can strike anyone-even people with perfect skin.
Why Misdiagnosis Is So Common (and Costly)
You’d think doctors would spot the difference. But they don’t always. A 2023 JAMA Dermatology study found that primary care doctors correctly diagnose these conditions only 52% of the time. Dermatologists? 85%. That gap matters. Why? Because they look alike. In fact, 68% of nail psoriasis cases show yellowing that’s nearly identical to fungal infection. So a patient comes in with a yellow, thickened toenail. The doctor sees fungus. Prescribes antifungal cream. The patient uses it for months. Nothing changes. The nail gets worse. Then they try oral pills. Side effects kick in. Still no improvement. By the time they see a specialist, they’ve spent 8 months and hundreds of dollars-and their nails are more damaged than before. On the flip side, fungal patients get misdiagnosed as psoriasis too. One patient on FootHealthForum wrote: “My dermatologist thought it was psoriasis and prescribed steroids. My nail got more brittle and started crumbling.” Steroids don’t kill fungus. They can even make it worse. The cost? In the U.S. alone, misdiagnosis leads to $850 million in unnecessary healthcare spending each year. That’s not just money. It’s time, stress, and worsening damage.
How Doctors Actually Diagnose This
If you’re seeing a dermatologist, here’s what should happen:- Clinical exam: They’ll look for pitting, oil spots, and how many nails are affected. If pitting is there, it’s almost certainly psoriasis.
- KOH prep: A tiny scraping from under the nail is mixed with potassium hydroxide. This dissolves skin cells, leaving fungal elements visible under the microscope. It’s fast, cheap ($15-$25), and 70-80% accurate.
- Fungal culture or PAS staining: If KOH is negative but suspicion remains, they’ll send a sample to a lab. Fungal cultures take 4-6 weeks but are 95% specific. PAS staining gives results faster and is 90% sensitive-meaning it catches most fungal cases.
There’s no single test that’s perfect. That’s why doctors use a combo. And if you’ve got psoriasis elsewhere? They’ll assume nail changes are psoriasis until proven otherwise.
Treatment: What Works (and What Doesn’t)
Fungal nails and psoriatic nails need completely different strategies. For fungal infections:- Oral antifungals: Terbinafine is the gold standard. Taken daily for 6-12 weeks. Clears the infection in 78% of cases after 12 weeks, confirmed by lab culture.
- Topical treatments: Efinaconazole (Jublia) or tavaborole (Kerydin). These work but take 9-12 months because nails grow so slowly-only 0.1 mm per day. You need to apply them daily, every day.
- Keep it dry: Fungus thrives in moisture. Wear breathable shoes. Change socks twice a day. Use antifungal powder. Humidity below 40% helps prevent recurrence.
- Corticosteroid injections: Injected directly into the nail matrix. Can show improvement in 8-12 weeks. Reduces inflammation and slows abnormal cell growth.
- Biologics: Drugs like secukinumab (Cosentyx) or ixekizumab. These target the immune system’s overreaction. In a 2022 CureTogether survey, 65% of patients saw major improvement after 24 weeks.
- Emollients: Thick ointments like petroleum jelly applied daily. Prevents cracking and separation. Avoid trauma-don’t pick, bite, or cut nails aggressively.
Never use antifungals for psoriasis. They won’t help. And never use steroids for fungus-they can make it spread.

What You Can Do at Home
You can’t diagnose yourself, but you can monitor:- Take monthly photos: Use the same lighting and angle. Compare them side by side. Changes in pitting, thickness, or color over time help your doctor spot patterns.
- Track symptoms: Did your nails change after a foot injury? That’s the Koebner phenomenon-trauma triggering psoriasis. Did they worsen after swimming or wearing boots? That’s fungus.
- Don’t ignore the smell: If your nail smells like old cheese or rot, it’s likely fungal. No smell? Could be psoriasis.
- Wear flip-flops in public showers: One simple habit cuts your risk of fungal infection by half.
The Future of Diagnosis
New tools are coming. Reflectance confocal microscopy-a non-invasive imaging tool-can see nail layers like an ultrasound. A 2023 Mayo Clinic study showed it correctly identified the condition in 92% of cases. Researchers are also studying the microbiome of the nail bed. Psoriasis nails have more Staphylococcus and less Cutibacterium. Fungal nails have high levels of Trichophyton DNA. In the next few years, a simple swab might tell you exactly what’s going on. AI is helping too. A 2024 study predicted a 22% drop in misdiagnosis by 2027 using apps that analyze nail photos. Imagine snapping a picture of your nail and getting a reliable assessment within minutes.Bottom Line
Don’t assume. Don’t guess. If your nails are changing, get them checked properly. Nail psoriasis and fungal infections are not the same. Treating one as the other doesn’t just waste time-it makes things worse. Look for pitting. Check for odor. Track how many nails are affected. And if you’ve had psoriasis before, don’t brush off nail changes as “just fungus.”The right diagnosis leads to the right treatment. And that’s the only way your nails will ever heal.
Can nail psoriasis turn into a fungal infection?
Yes. Nail psoriasis damages the nail structure, creating cracks and gaps where fungi can enter. Studies show that 4.6% to 30% of people with nail psoriasis develop a secondary fungal infection. This is called a superinfection. It’s not that psoriasis becomes fungus-it just makes it easier for fungus to take hold.
Is nail psoriasis contagious?
No. Nail psoriasis is an autoimmune condition, not an infection. You can’t catch it from someone else. Fungal nail infections, however, are contagious. They spread through shared towels, shoes, or public showers. That’s why it’s important to know which one you have.
Why do antifungal treatments fail for psoriasis?
Because the root cause isn’t fungus. Antifungals kill fungi, but they don’t stop your immune system from attacking your nail matrix. If your nails are thickening and lifting due to psoriasis, antifungals have nothing to target. They won’t reduce inflammation or slow abnormal cell growth. That’s why they don’t work-and why using them can delay the right treatment.
Can stress make nail psoriasis worse?
Yes. Stress is a known trigger for psoriasis flare-ups, including nail changes. Emotional stress, physical trauma, or even illness can activate the immune system and worsen nail pitting, thickening, or separation. Managing stress through sleep, exercise, or mindfulness can help reduce flare frequency.
How long does it take for a nail to grow back normally?
Fingernails grow about 3.5 mm per month and take 6 months to fully replace. Toenails grow slower-about 1.6 mm per month-and can take 12 to 18 months to grow out completely. That’s why treatment takes so long. Even after the infection or inflammation is gone, you have to wait for the damaged nail to grow out and be replaced by healthy tissue.





Kenneth Jones
March 24, 2026 AT 15:39Mihir Patel
March 25, 2026 AT 10:18Grace Kusta Nasralla
March 25, 2026 AT 18:16Anil Arekar
March 27, 2026 AT 14:21Elaine Parra
March 28, 2026 AT 07:59Amber Gray
March 29, 2026 AT 22:46Danielle Arnold
March 30, 2026 AT 08:13Blessing Ogboso
March 30, 2026 AT 14:11florence matthews
March 31, 2026 AT 16:22Kevin Y.
April 1, 2026 AT 18:49Raphael Schwartz
April 2, 2026 AT 17:48Aaron Sims
April 2, 2026 AT 21:58peter vencken
April 3, 2026 AT 21:05Chris Crosson
April 4, 2026 AT 03:09Linda Foster
April 5, 2026 AT 10:54